Greater Trochanteric Bursitis: Why Cortisone Keeps Wearing Off (And What Lasts Longer)
Greater trochanteric bursitis is one of the most common causes of lateral hip pain, particularly in women over 40 — and one of the most frequently mismanaged. It mimics hip arthritis closely enough that it's often misdiagnosed, and its standard treatment, the cortisone injection, tends to provide temporary rather than lasting relief. Understanding why requires a closer look at what's actually happening in the tissue.
What the Bursa Is and What Goes Wrong
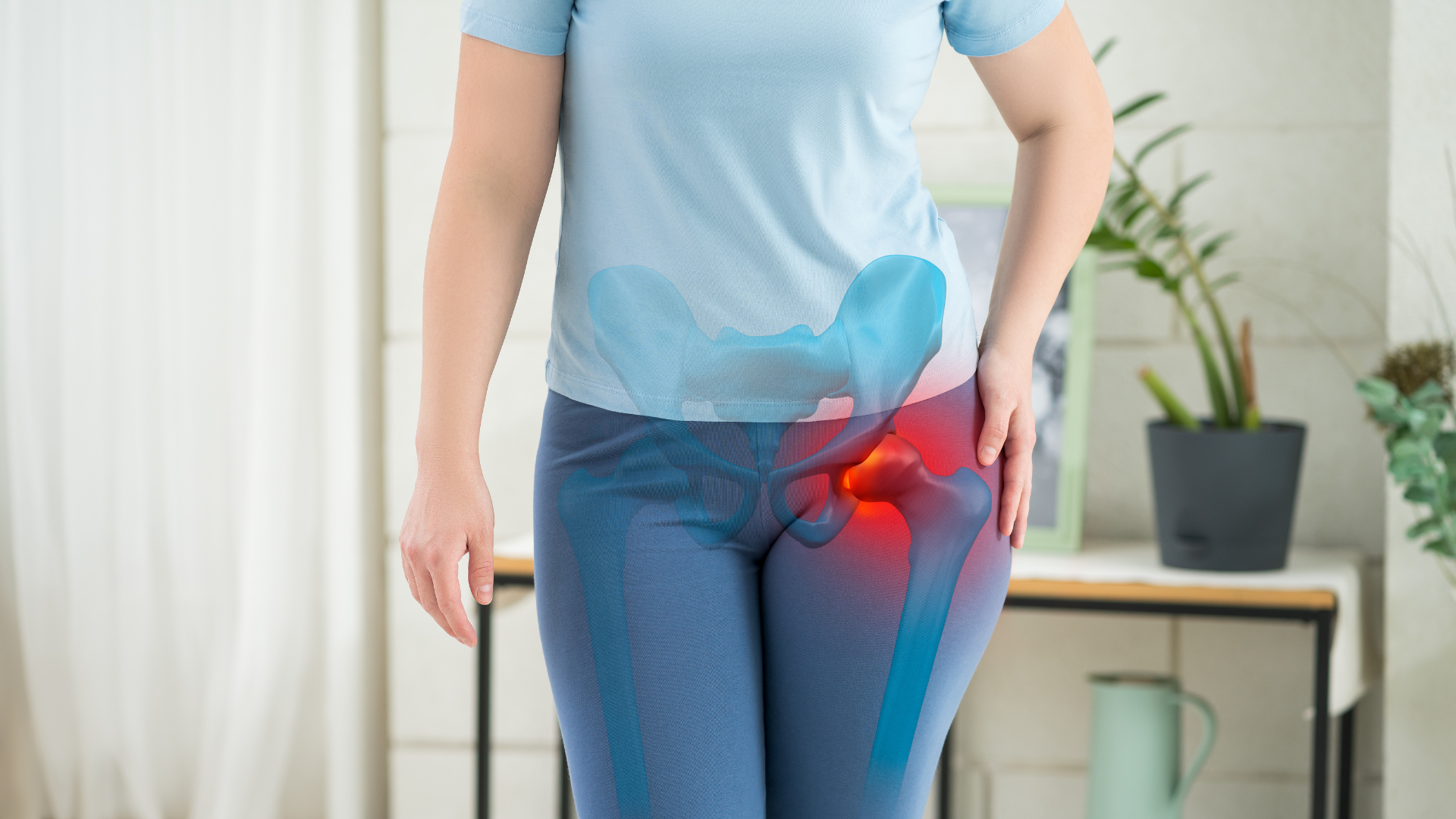
The greater trochanteric bursa is a fluid-filled sac located over the greater trochanter — the bony prominence on the outer side of your hip that you can feel when you press on the widest part of your hip. Its function is to reduce friction between the iliotibial band and gluteal tendons as they pass over the trochanter during movement.
When the bursa becomes inflamed — from repetitive friction, sudden increase in activity, direct trauma, or altered hip mechanics from an adjacent problem like lumbar spine pathology or IT band tightness — it swells and becomes a significant pain generator. The classic symptoms are pain directly over the greater trochanter, worsening with lying on the affected side, and pain with activities that compress or load the lateral hip like climbing stairs, crossing legs, or rising from a low seat.
Why Cortisone Wears Off
Cortisone is a potent anti-inflammatory agent. Injected directly into the bursa, it can produce rapid and significant pain relief by suppressing the inflammatory response. For many patients, this relief lasts four to eight weeks.
But cortisone doesn't change the mechanical or biological factors that caused the bursitis to develop. If the underlying tissue pathology — tendon degeneration, IT band tension, altered hip mechanics, poor local circulation — hasn't been addressed, the inflammatory cycle restarts once the cortisone clears the system.
Repeated cortisone injections are associated with their own risks over time, including tendon weakening and local tissue atrophy. Most orthopedic guidelines now recommend limiting injections to two to three in the same site.
What SoftWave Changes
SoftWave Therapy for greater trochanteric bursitis targets the underlying tissue pathology rather than simply suppressing the inflammatory response.
The acoustic waves stimulate healing in the gluteal tendons that often develop concurrent tendinopathic changes alongside the bursitis — a condition called gluteal tendinopathy that is now understood to be a major contributor to lateral hip pain. Angiogenesis restores blood supply to the chronically irritated tissue. Stem cell recruitment supports repair of the tendon matrix. Anti-inflammatory signaling at the cellular level interrupts the chronic inflammatory cycle without the side effects associated with repeated steroid use.
For many patients, SoftWave provides pain relief comparable to cortisone in duration and superior in sustainability, because it addresses the tissue-level causes of the condition rather than suppressing its symptoms.
📞 Call 314-252-0345 to schedule a SoftWave Discovery Session. We come to your home.